Please type the text you see in the image into the text box and submit
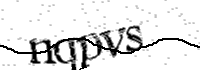
[ Refresh the page to generate a new image. ]
If you get here while trying to submit a form, you may have to re-submit the form.
Access to this domain may need the browser to have javascript and cookie support enabled.